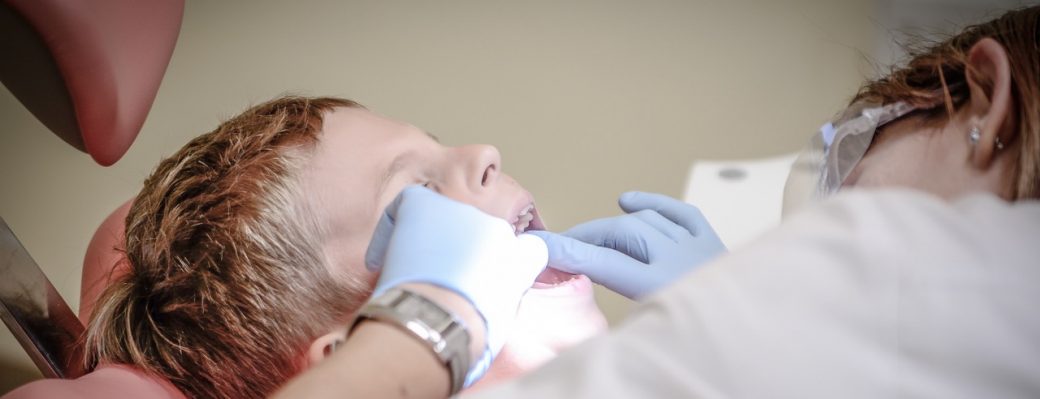
Are you looking for another nonsurgical procedure to treat your chronic back pain? Or does your chiropractor recommend your condition for manipulation under anesthesia? If your chronic pain symptom does not fix by nonsurgical care, other conservative treatment like manipulation under anesthesia can be performed on you. However, there are some situations this procedure is not applicable. Doctors can schedule sessions of manipulation under anesthesia for pain, depending on the degree of your condition.
The Concept of Manipulation Under Anesthesia
Manipulation under anesthesia (MUA) is a noninvasive extending and manipulative procedure. The doctor performs MUA to relieve chronic pain and pain that have not reacted to long-term conservative care.
MUA separates adhesions interior scar tissue that can result from injury or medical procedure and may help reestablish a more typical scope of movement and diminish pain. Usually, this treatment is for neck, joint, back pain, and other chronic pain like muscle spasms and long-lasting pain syndromes.
Adhesions can develop around spinal joints and nerve roots and within encompassing muscles, bringing about confined development, restricted flexibility, and pain.
It is speculated that one of the causes of chronic pain, like tight muscle spasms, might be the overabundance of scar tissue that developed in or close to joints from former injuries and surgical procedures. Additionally, these scar tissues called fibrous adhesions might result in chronic inflammation for nearby systems, such as muscles or nerves. This condition may also cause stiff joints and pain when moving.
In case spinal joints are too excruciating even to consider moving for manual manipulation process or physical therapy, a doctor may suggest manipulation under anesthesia. Because of the anesthesia, the standard guarding components of the muscles unwind. Doctors can put the joints through scopes of movement that would otherwise not be possible with the conscious patient. These manipulations accomplished under anesthesia aim to stretch or separate the excess scar tissues to result in less confrontation and aggravation.
Manipulation Under Anesthesia for Spinal Pain
Doctors recommend spinal manipulation under anesthesia (MUA) to alleviate chronic pain from the neck and back when other techniques did not work. The method includes sedating the patient and doing spinal stretches and exercises that would somehow be excessively painful because of muscle spasms or unnecessary scar tissue. Even though MUA is not as popular as systematic manual manipulation, it has been around for quite a long time in several forms.
How The Doctors Performed The Spinal Manipulation Under Anesthesia
Spinal MUA applies a combination of manipulations to stretch out the scar tissue around the spine and surrounding tissue. These techniques include articular and postural moves, definite short-lever spinal manipulations, and passive stretches. Chiropractors or osteopaths are typically the ones who can accomplish this combination. Notwithstanding, the method’s details can change essentially from clinic to clinic since the business has not yet established proper norms for the procedure.
Moreover, spinal manipulation under anesthesia can be completed in a hospital by qualified doctors with special training and certification for the practice. A group approach with numerous doctors and associate is necessary to have a secure and effective outcome.
There are different types of anesthesia for manipulation procedures. These include:
- General anesthesia makes the patient entirely unconscious for the whole process.
- Slight sedation makes the patient conscious of the treatment yet not experiencing pain nor prone to recall the procedure.
- Local anesthetic can numb one specific area, like one or two most painful joints, permitting the patient to stay awake for the process.
Generally, one meeting of spinal MUA consumes less than an hour. At times the system can be just about as short as 10 or 15 minutes. However, it may repeat on consecutive days to accomplish a comparable degree of help with minor soreness from the technique itself.
Qualified Professionals for Spinal Manipulation Under Anesthesia
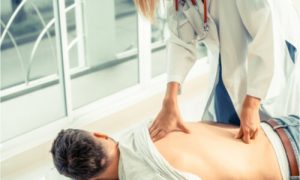 The medical group who can accomplish spinal MUA regularly incorporates:
The medical group who can accomplish spinal MUA regularly incorporates:
- The main chiropractor or other specialists who execute the manipulation
- The co-attending specialist who is a primary assistant and certified in manipulation under anesthesia
- Anesthetist responsible for regulating the anesthesia and observing the patient
- Nurses and other subordinates who may help all through the process
Varieties of the medical group’s size and mastery can shift from clinic to clinic. For instance, some teams may be driven by a physiatrist or orthopedic surgeon instead of a chiropractor.
Benefits of Manipulation Under Anesthesia Treatment
Some individuals with back pain react well to exercise, physical therapy, or chiropractic manipulation. However, their relief may only experience for days or weeks. At times, MUA is more effective in improving the scope of movement and easing pain. Manipulation under anesthesia can be more practical and secure than intrusive techniques, such as spine surgical procedures.
Some possible benefits the patient can get from manipulation under anesthesia include:
- Stretching or breaking up excessive scar tissue both in and around the spinal joints
- Reducing chronic muscle spasm
- Reducing the hypersensitivity of harmed zones to empower the patient to proceed with various treatments like traditional manual manipulation, physical therapy, or exercise
- Stretching shortened muscles, tendons, and ligaments
- Diminishing pain associated with fibromyalgia
- Dismissing pain and transmitting indications from harmed intervertebral plates
Other advantages from spinal MUA have additionally been accounted for relief from cervicogenic headache coming from the neck. Also, manipulation under anesthesia is recognized and covered by most insurance and employees’ compensation.
How to Determine If Manipulation Under Anesthesia is The Right Treatment?
Manipulation under anesthesia is not for all individuals with back pain. Instead, the doctor prescribes MUA to people who meet the technique’s selection criteria. Like some other treatment suggested, the doctor considers the patient’s clinical history, indications, past medicines, and effectiveness level.
Moreover, the doctor makes a physical and neurological examination other than talking with the patient about their complete medical history. Test outcomes support the doctor in certifying the patient’s finding and deciding whether MUA can help ease and other side effects. These include:
- X-ray
- MRI or CT scan
- A musculoskeletal sonogram, an ultrasound imaging that applies sound waves to deliver pictures of muscles, ligaments, tendons, and joints in the body
- Electrocardiogram (EKG) is a test that examines for issues with the heart’s electrical movement
- Nerve conduction velocity (NVC) test is a test to check how quickly electrical signals travel through a nerve
- Pregnancy test for ladies of childbearing age
When Spinal Manipulation Under Anesthesia May Be Considered
Spinal MUA considers to be an elective type of treatment for patients with at least one of the following indications after conservative care has demonstrated ineffective:
- Chronic sprain or strain
- Chronic disc conditions
- Persistent neck, mid or lower back pain
- Chronic muscle discomfort and aggravation
- Chronic muscle spasm or recurring intense spasm
- Painful, restricted range of motion
- Nerve compression syndrome or pain radiating into an arm or leg
- Cervicogenic headache or pain from the neck that goes up into the head
- Failed back surgery syndrome
- Fibrous adhesion
- Fibromyalgia
Generally, doctors usually consider spinal MUA when conventional manipulation is safe and beneficial. However, patients cannot endure it because of high levels of pain and decreased range of motion.
When to Abstain from Spinal Manipulation Under Anesthesia
 The doctors screen the patient when considering spinal MUA. He or she will check for any conditions that would make the body far-fetched to securely deal with the procedure’s extensive stretching, high-speed moves, and medications. Some particular contraindications for spinal MUA incorporate:
The doctors screen the patient when considering spinal MUA. He or she will check for any conditions that would make the body far-fetched to securely deal with the procedure’s extensive stretching, high-speed moves, and medications. Some particular contraindications for spinal MUA incorporate:
- Bone fracture in the region to be manipulated, like spine, pelvis, arm, or leg
- Any cancer
- Osteomyelitis or vertebral bone infection
- Spinal cord compression with long-plot signs
- Acute inflammatory arthritis, spinal osteoporosis, or other bone weakness
- Cauda equina syndrome
- Morbid obesity
- Acute gout attack
- Neurological problems, together with uncontrolled diabetes
- Advanced age
Numerous different conditions could likewise make it desirable to delay or keep away from spinal MUA like pregnancy or incapacity to receive anesthesia.
Post-Procedure Care
The patient can start the post-procedure treatments right after the doctor completed the spinal MUA. These medications are typically set in the doctor’s facility and may incorporate:
Cold packs
Using ice or a cold pack can help lessen irritation, inflammation, and pain. It would help if you took care to examine the skin occasionally to prevent tissue harm. Typically, 10 or 20 minutes are the appropriate periods to apply a cold pack on the skin.
Massage
Massaging the soft tissues is a necessary part of post-procedure care. It improves circulation and relaxation of the muscles and joints. Some of the time, doctors apply cold treatment combined with massage, called ice massage.
Electrotherapy
Typically, doctors use a battery-powered gadget that will connect to adhesive electrodes set on the skin. This device will send electrical heartbeats to the problem zone and may help diminish pain. Transcutaneous electrical nerve stimulation (TENS) is the most popular type of electrotherapy.
Ultrasound
This treatment is a type of mechanical energy that uses mechanical vibration known as ultrasound. Ultrasound therapy may give gentle vibrations into the skin and various soft tissues to expand blood circulation and possibly lessening pain.
After the spinal MUA technique, the patient needs a relative or friend to send him home to rest. After receiving anesthesia, the doctor will typically recommend the patient to try not to drive for 24 hours.